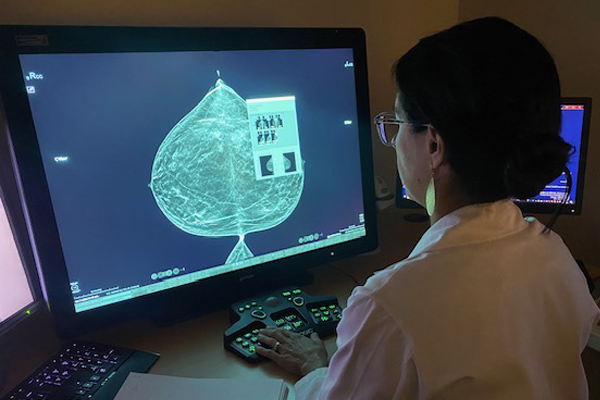
Dr. Emily Stone discusses the importance of routine screening for breast cancer and what to expect if you are called back for more imaging
Breast cancer is the most common cancer (aside from skin cancers) among American women. One in 8 women will have breast cancer by the time she is 75. For the average woman, there is about a 12% lifetime risk. Yet if detected early, when the cancer is localized (hasn’t spread beyond the breast), the 5-year relative survival rate of breast cancer is 99%. That means women who have been diagnosed at this stage are 99% as likely to live for at least five years as women who do not have breast cancer. I’d like to discuss how and when to begin screening for breast cancer and what it means to be called back for more imaging if the results don’t come back as “normal.” Staying on top of your annual screenings is even easier with our new mammography suite at VPFW St. Francis.
Why it’s important to screen for breast cancer every year
You may not realize that 75% of women diagnosed with breast cancer have no special or identifiable risk factors. Luckily, we have mammography, the primary screening tool we use to look for breast cancer in women who don’t have any signs or symptoms. Mammograms use a small amount of radiation (X-ray) to give us a view of the breast from the inside.
The goal of mammography is to reduce deaths due to breast cancer by detecting the disease early when treatment is more effective and less harmful. The risk of death from breast cancer is decreased by 30-48% with routine mammographic screening.
What age should women begin annual mammograms?
The American College of Obstetrics and Gynecology and the American College of Radiology recommend yearly screening mammograms starting at age 40. Breast cancer grows more rapidly in women in their 40s and early 50s.
A personal family history of breast cancer means you may start screenings earlier. For women with a first degree relative with breast cancer (mother or sister), screening mammograms should begin ten years prior to your relative’s age at diagnosis. For women who carry BRCA-1 or BRCA-2 gene mutations (the most common cause of hereditary breast cancer), annual mammograms should begin at 25. Breast MRI also may be used for screening in women who carry the BRCA gene mutation.
Women (or girls) who have been exposed to chest radiation (likely to treat another cancer) before age 40 should start screening mammograms and consider a screening breast MRI eight years after radiation treatment.
What are the odds of finding something concerning?

Out of 100 women receiving their annual screening mammogram, 90 will be told everything looks normal. Ten will be “called back” for more evaluation (additional mammographic views and often an ultrasound).
Of the women who are called back, about 50% will have normal results, about 15% will be advised to have a biopsy, and 2-5% will be diagnosed with breast cancer.
3D mammograms, which take multiple X-ray images from different angles to create a 3D image of the breast, are now routine. They offer improved imaging and reduce the rate of women being “called back” for further imaging.
What to Know About the COVID-19 Vaccine and Mammograms
Of course, COVID-19 rears its head into our breast screening plans. Due to the increased likelihood of axillary adenopathy (enlarged armpit lymph nodes) from COVID-19 vaccination, the timeline for screening mammograms for those about to be vaccinated has been adjusted. Our radiology colleagues recommend having your mammogram prior to your COVID-19 vaccine or 6 weeks after your vaccination is complete, when any adenopathy from the vaccine will likely be resolved. This recommendation is to prevent false positive readings on mammograms.
VPFW Now Offers Mammograms at our St. Francis Location!
VPFW’s St. Francis office is excited to have opened a new mammography suite this winter. St. Francis joins our Midlothian Turnpike, West Creek, and Prince George locations in offering mammograms that are read by our colleagues with Radiology Associates of Richmond.
With mammography on site, planning for your annual exam and mammogram together could not be easier! Our phone staff is ready to answer questions about scheduling, especially regarding the COVID-19 vaccine. We are also happy to discuss specific risk-related questions. Learn more on our mammography page.
To make an appointment with an OB/GYN provider at one of our Richmond, VA, locations, call VPFW at 804-897-2100 or message us to schedule online.
Last updated March 13, 2026