Hollie Jones, N.P., discusses how triple negative breast cancer differs from other breast cancers, its distinct risk factors, and what you can do for prevention and early detection.
TL;DR: Triple negative breast cancer (TNBC) is an aggressive form of breast cancer that lacks three common hormone receptors, making it harder to treat; but early detection and ongoing research offer hope.
- TNBC lacks estrogen, progesterone, and HER2 receptors.
- It does not respond to common hormone or HER2-targeted treatments.
- TNBC grows and spreads more quickly than other types.
- Chemotherapy is the primary treatment, but new therapies are emerging.
- TNBC has a distinct risk factor profile vs. overall breast cancer
- Early detection improves prognosis—know your risk, schedule your annual screening mammogram, and practice breast self-awareness
What is triple negative breast cancer (TNBC), and why is it considered more challenging to treat than other types? In essence, TNBC doesn’t respond to most of the common treatments used to treat other breast cancers.
However, there are options when it comes to treatment approaches for triple negative breast cancer, and there is hope if you are diagnosed. Continue reading to learn the basic facts about TNBC, its unique risk factor profile, and what you can do to put yourself in the best position for prevention, early detection, and successful treatment.
Understanding Triple Negative Breast Cancer
Triple negative breast cancer is a subtype of breast cancer. It’s unique in that it does not express the three most common markers found in most other breast cancers:
- Estrogen receptors: Proteins on some breast cancer cells that allow them to grow in response to the hormone estrogen.
- Progesterone receptors: Proteins that allow breast cancer cells to grow in response to the hormone progesterone.
- Human Epidermal Growth Factor Receptor 2 (HER2) receptors: proteins that help breast cancer cells grow and divide quickly when there are too many of them on the cell surface.
Triple negative breast cancer gets its name because it tests negative for each of these three key proteins that are typically tested for in a breast cancer tumor to determine its subtype. That means TNBC does not respond to common hormonal therapies (like tamoxifen) or HER2-targeted treatments (like trastuzumab).
Triple negative breast cancer also differs from other breast cancers in that it is often considered a more aggressive form of cancer. In simpler terms, it grows and spreads faster than other types and is more likely to come back after treatment.
Why TNBC Is Harder to Treat
Treating triple negative breast cancer can be challenging because without these three receptors, there is a lack of targeted therapies available. As a result, doctors must rely heavily on chemotherapy treatments. Chemotherapy affects the whole body and can come with significant side effects.
TNBC is also more often diagnosed at later stages. For instance, stage 3 triple negative breast cancer may have already spread to nearby lymph nodes or tissues. That can complicate treatment options.
With that said, there is hope on the horizon. Researchers are actively exploring new triple negative breast cancer therapies, including immunotherapy and PARP inhibitors.
Triple Negative Breast Cancer Prognosis and Survival Rate
Because of its aggressive nature, the triple negative breast cancer prognosis can feel daunting. However, outcomes can vary significantly depending on the stage at diagnosis and how well the cancer responds to treatment.
For early-stage TNBC, the triple negative breast cancer survival rate is similar to that of other forms of breast cancer. With that said, survival rates decline if the cancer is found at a later stage or recurs after initial treatment.
It’s important to remember that every person’s experience is unique. Advances in research are leading to better therapies and more hope for those diagnosed with TNBC.
Triple Negative Breast Cancer’s Unique Risk Factor Profile
A new research study analyzing 33 studies on breast cancer risk factors has found that the risk factor profile of triple negative breast cancer differs slightly from the risk factor profile of other breast cancers. The studies included nearly 11,000 women diagnosed with triple-negative breast cancer.
Factors linked to higher risk for TNBC
The research results showed the following risk factors had statistically significant links to a higher risk for triple negative breast cancer specifically:
- Having a family history of breast cancer
- Using birth control pills for more than 10 years
- Having dense breast tissue
Age is another differentiating factor of triple negative breast cancer. TNBC is more common in premenopausal women and women under 50 than other types of breast cancer. In patients older than 70, other types of breast cancer are more common than TNC.
Factors linked to lower risk for TNBC
The results also showed two risk factors with statistically significant links to a lower risk for triple negative breast cancer specifically:
- Having your first period at age 14 or older
- Breastfeeding
- Being older than age 30 when giving birth for the first time
On the contrary, studies have found that women who were under age 30 when giving birth to their first child have a lower risk of other types of breast cancer.
Know Your Risk
It’s important to talk with your doctor about your personal risk factors for triple negative breast cancer in addition to overall breast cancer. While many factors are out of our control, there may be things you can do to lower your risk.
For example, if you have been taking oral contraception for close to 10 ten years, you and your provider could discuss alternative birth control options such as injections, a vaginal ring, a patch, an IUD, or a more permanent option.
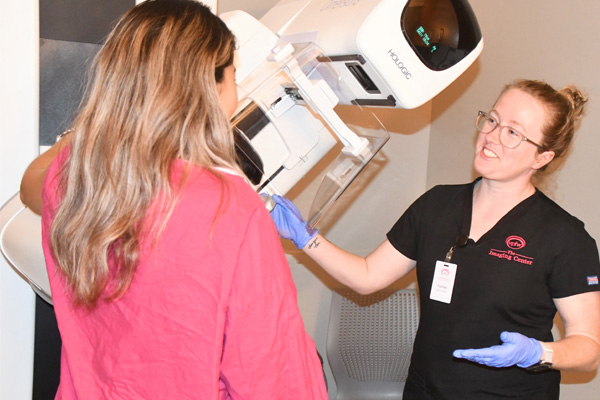
Make Early Detection a Priority
Being proactive about scheduling annual screening mammograms and practicing breast self-awareness are crucial for the detection of all types of breast cancer. However, since TNBC often affects women who are younger than age 40, which is the recommended age to begin screening mammograms for most women, self-breast awareness – becoming familiar with your breasts so that you notice any changes – is extremely important for women under 40.
If you have dense breast tissue, which is one of the risk factors for TNBC, you and your doctor should discuss supplementing your annual screening mammograms with annual breast MRI’s. It’s more difficult to detect breast cancer (of any type) in dense breast tissue on a mammogram. Monthly self-breast exams are also strongly encouraged for women with dense breast tissue. Learn more in our blog post by radiologist Dr. Nicole Kelleher, What a Radiologist Wants you to Know About Mammograms.
These approaches can help women catch TNBC and other types of breast cancer as early as possible. Detection in early stages usually means the cancer will require a less aggressive course of treatment. While TNBC research and treatments are improving, it’s still true that the sooner treatment begins, the better the prognosis.
The team at VPFW can help you make your breast health a priority. Schedule your annual screening mammogram at one of four VPFW locations today.
